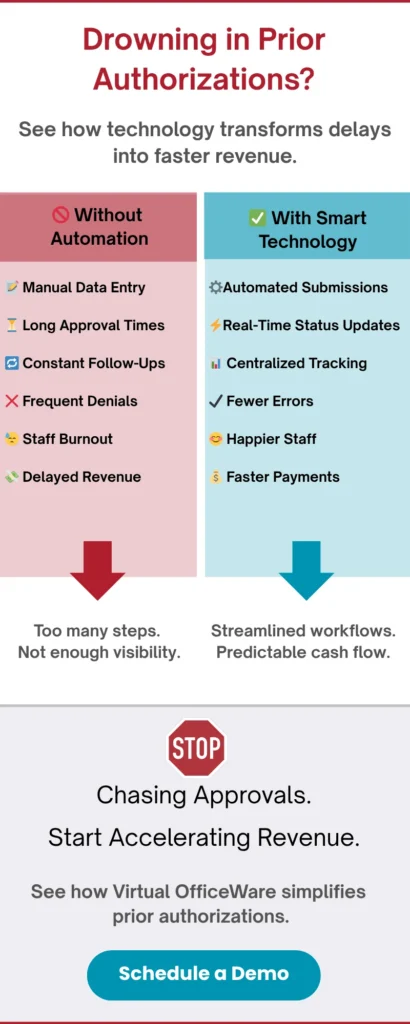
Drowning in Prior Authorizations? Cut Delays and Protect Revenue in 2026

Why Are Prior Authorization Delays Still Hurting Healthcare Practices?
Many healthcare physicians feel like they are drowning in prior authorizations, leading to significant workflow slowdowns.
Prior authorizations were designed to ensure proper care. However, today they often create delays that disrupt both patient care and revenue cycles.
Staff spend hours managing prior authorization workflows. Patients wait longer than expected. Meanwhile, your healthcare revenue cycle slows down.
The truth is that most practices don’t realize how much revenue is slipping through the cracks.
Even worse, delays in prior authorization processing can often lead to claim denials. And denied claims directly impact your practice’s cash flow.
So, what’s causing these prior authorization challenges?

- Manual prior authorization processes are still common
- Insurance payer requirements change frequently
- Staff are stretched too thin managing administrative tasks
- Communication gaps lead to costly authorization errors
As a result, your team feels overwhelmed. Burnout increases. Productivity drops. Revenue becomes unpredictable.
However, the good news is this: healthcare technology in 2026 is transforming prior authorization management.
How Can Technology Improve Prior Authorization Workflows?
1. Automating Prior Authorization Processes
First, automation reduces the need for manual data entry in prior authorization workflows. Instead of repeating the same steps, systems auto-fill required information.
This significantly improves prior authorization efficiency.
Additionally, automation tools can:
- Submit prior authorization requests electronically
- Track authorization status in real time
- Flag missing or incorrect information before submission
Because of this, errors decrease and approval times improve. Staff can shift focus to higher-value tasks within the revenue cycle management process.
2. Real-Time Eligibility and Authorization Checks
Next, modern systems verify payer requirements instantly. This helps prevent errors before submitting prior authorization requests.
Without real-time checks, incomplete submissions often lead to delays or denials.
With these tools, your team can:
- Avoid missing authorization requirements
- Reduce back-and-forth with payers
- Accelerate approval timelines
For example, integrated EHR and prior authorization software can alert staff during scheduling or patient intake.
Learn more about healthcare technology trends from trusted sources like HealthIT.gov and HFMA.
3. Centralized Prior Authorization Tracking
Another common issue is fragmented communication. Emails, faxes, and phone calls create confusion across teams.
However, centralized dashboards improve prior authorization tracking and visibility.
With a unified system, your team can:
- Monitor every authorization request from start to finish
- Set automated reminders for follow-ups
- Access payer responses in one place
As a result, your prior authorization workflow becomes more organized and efficient.
How Do Prior Authorization Delays Impact Revenue Cycle Performance?
Fewer Denials and Faster Reimbursements
When prior authorizations are accurate and timely, claims are more likely to be approved on the first submission.
This leads to:
- Fewer claim denials related to authorization
- Faster insurance reimbursements
- Improved healthcare cash flow
In contrast, inefficient prior authorization management often results in preventable revenue loss.
Lower Administrative Costs
At the same time, automation reduces the administrative burden. Staff spend less time handling repetitive authorization tasks.
Consequently, practices improve operational efficiency and reduce overhead costs.
Better Patient Experience
Patients feel the impact of authorization delays. Long wait times can lead to frustration and dissatisfaction.
On the other hand, faster prior authorization approvals result in:
- Quicker access to care
- Better communication with patients
- Higher satisfaction rates
And satisfied patients are more likely to return and recommend your practice.
How Can Your Practice Improve Prior Authorization Management in 2026?
Step 1: Evaluate Your Current Prior Authorization Workflow
First, assess where delays occur in your current authorization process. Identify manual steps and inefficiencies.
Understanding these gaps is critical for improving your revenue cycle performance.
Step 2: Invest in Prior Authorization Technology
Next, implement solutions that integrate with your existing systems. Look for features that support:
- Automated prior authorization submissions
- Real-time eligibility verification
- Centralized tracking and reporting
Explore Virtual OfficeWare’s Revenue Cycle Management services to streamline your workflow.
Step 3: Partner with Revenue Cycle Experts
Finally, working with experienced partners can improve outcomes faster. Instead of managing everything internally, leverage proven expertise.
Virtual OfficeWare provides solutions designed to:
- Reduce prior authorization delays
- Improve clean claim rates
- Optimize healthcare revenue cycle performance
Learn more by visiting Virtual OfficeWare.
Why Is Prior Authorization Optimization Critical in 2026?
![]()
Regulatory requirements continue to evolve. Insurance payers are becoming more complex. As a result, prior authorization compliance is more challenging than ever.
Because of this, outdated processes cannot keep up.
In 2026, successful practices rely on:
- Speed in prior authorization approvals
- Accuracy in submissions
- Efficiency across the revenue cycle
Without the right tools, healthcare organizations risk falling behind.
Frequently Asked Questions
What is prior authorization in healthcare?
Prior authorization is a process where insurance payers require approval before certain treatments or services are provided.
Why do prior authorization delays happen?
Delays often occur due to manual processes, missing information, and changing payer requirements.
How does technology reduce prior authorization delays in healthcare?
Technology reduces prior authorization delays by automating submissions, verifying requirements in real time, and minimizing errors before claims are sent. As a result, approvals happen faster, administrative workload decreases, and revenue cycle efficiency improves.
How do prior authorizations impact the revenue cycle?
Inefficient prior authorization processes can lead to claim denials, delayed payments, and reduced cash flow.
Should healthcare practices outsource prior authorization management?
Outsourcing can improve efficiency, reduce staff workload, and enhance revenue cycle performance.
Ready to Reduce Prior Authorization Delays and Improve Cash Flow?
You do not have to keep struggling with inefficient prior authorization workflows, delayed reimbursements, and staff burnout.
Instead, you can streamline your processes, improve revenue cycle performance, and enhance patient satisfaction.
Schedule your personalized demo today and see how much revenue your practice can recover.